STRIDOR IN AN INFANT WITH CUTANEOUS HAEMANGIOMA: A CASE REPORT
Okolie EI¹*, Taiwo G², Nebeife PC³, Ekedigwe SO³
¹Department of Obstetrics and Gynaecology, Enugu State University of Science and Technology Teaching Hospital, Enugu.
2Newham University Hospital, Glen Road, Plaistow, London.
3Cedarcrest Hospitals Limited, Niger State Branch.
*Correspondence: Dr. Emmanuel Ikechukwu Okolie; +2348133704100; okolieemmanuel8@gmail.com
Abstract
Abstract
Background: Airway haemangiomas are rare but can be life-threatening during the proliferative phase. They are often misdiagnosed as common respiratory conditions. The presence of cutaneous haemangiomas, particularly in the “beard” distribution, should raise suspicion of airway involvement. Limited facilities and financial constraints may hinder further investigations for confirmation. Propranolol has emerged as the first-line treatment for infantile haemangiomas, including airway involvement, offering rapid regression and improved outcomes.
Case Presentation: A three-month-old infant presented with recurrent respiratory distress, biphasic stridor, and raised cutaneous haemangiomas involving the posterior neck, left lower jaw, left buccal area, and left border of the tongue. The infant had been misdiagnosed and previously treated for bronchiolitis. The presence of facial cutaneous haemangiomas led to suspicion of airway involvement. A diagnosis of infantile haemangioma in the “beard” distribution with upper airway involvement was made, and the infant was treated with intranasal oxygen, intravenous hydrocortisone, and oral propranolol. The patient showed a modest response to treatment, with a reduction in respiratory distress and stridor, as well as marked reduction in cutaneous lesions.
Conclusion: A high index of suspicion is needed, especially in infants presenting with respiratory distress and associated cutaneous haemangiomas. Propranolol has revolutionized the treatment of infantile haemangiomas and should be considered as the first-line therapy. However, careful monitoring for potential side effects is essential. Improved awareness and accessibility to appropriate care are essential to optimize outcomes, especially in resource-limited settings.
Keywords: Stridor, Cutaneous haemangioma.
Cite this article: Okolie EI, Taiwo G, Nebeife PC, Ekedigwe SO. Stridor in an infant with cutaneous haemangioma: a case report. Yen Med J. 2023;5(2):75–78.
INTRODUCTION
Infantile haemangiomas (IH)s are the most frequently encountered benign vascular tumors during infancy and present in 4% to 5% of the population.1-3 They appear as bright red, protuberant, compressible, sharply demarcated lesions that may be found in any part of the body.¹
The exact etiology of IH is unknown but studies have demonstrated risk factors such as female gender, multiple gestation, preterm birth, progesterone therapy, family history of IH, low birth weight (every 500g decrease in birthweight increases the risk by 40%), Caucasian race, in vitro fertilization, and maternal age greater than 30 years.3-6
In most cases, infantile haemangiomas are not present at birth, although they may be present only as lesions characterized by an area of pallor, telangiectasias, or duskiness.2,4,6,7
They however become evident in a period of 1-2 weeks from birth and then go through a natural cycle that consists of three phases: the rapid proliferation phase (with the most rapid growth between 5.5 – 7.5 weeks), the plateau phase and the slow involution phase. At around 9 months on the average, the IH has reached its maximum size, and by the age of 4 years, regression is completed in about 90% of cases, mostly without leaving significant scarring.2,4,6
Cutaneous infantile haemangiomas can be localized, segmental or indeterminate. Segmental haemangiomas appear in areas of the body that correspond to a portion of a developmental segment or broad anatomical territory. They are often plaque-like with linear or geographic configurations possessing a higher risk of complications.6 Segmental haemangiomas are at increased risk of being associated with life threatening lesions such as obstructing IHs of the airways.2,3
Airway haemangiomas typically involve the subglottis in an entity known as subglottic haemangioma (SGH) which represents 1.5% of the congenital laryngeal abnormalities.3,7 Almost 50% of them are associated with cutaneous haemangiomas present in the “beard” or S3 distribution. This distribution includes the preauricular skin, mandible, lower lip, chin, and/or anterior neck.7-9
Subglottic haemangioma has the potential to cause life threatening complications in the newborn period with biphasic stridor, often exacerbated by crying and upper respiratory tract infections as the most common presenting symptoms.5 Symptoms often present before 4-6 months of age with the natural history of the disease characterized by progressive airway obstruction during the proliferative phase followed by resolution of symptoms during the involution phase.5,10
The diagnosis of SGH is made based on clinical presentation of the child.8 The presence of cutaneous large haemangiomas in the beard distribution along with stridor/respiratory distress should generate a high index of suspicion of SGH.7 However, confirmation is achieved by visualization of the lesion during laryngobronchoscopy.8
Current treatment modalities for problematic haemangiomas include pharmacotherapy, laser therapy and surgery.1 Since it’s discovery in 2008 by Leaute-Labreze et al, propranolol is now the first line treatment for all forms of infantile haemangiomas and ended the era of glucocorticoids as the gold standard.1,2,4,7 The mean estimate of expected clearance for oral propranolol was 95% in a meta-analysis, which was superior to other interventions.3 Most studies recommend dosing at 2 to 3mg/kg per day of oral propranolol for a duration of 6 months.3 However, when used, systemic corticosteroids are frequently dosed between 2-3mg/kg per day of oral prednisolone for an average duration of 6 months.2
This study aims to present a case that emphasizes the need for high index of suspicion of airway haemangiomas in infants presenting with stridor or respiratory distress associated with the presence of facial cutaneous haemangiomas.
CASE PRESENTATION
A three-month old girl baby presented to the Emergency Department with a history of recurrent noisy breathing, cough and difficulty with breathing of three weeks duration.
The first two episodes had been misdiagnosed as bronchiolitis and managed with systemic steroids after which she was discharged in stable conditions.
The current episode, being the third, started a day prior to presentation, and eight days following her last discharge. Her symptoms increased when child was kept in supine position as well as while suckling on the breast or crying.
There was no fever, associated change in voice or drooling of saliva. She was the sixth child delivered at term via spontaneous vaginal birth to non-consanguinous parents. Parents could not recall her birthweight. Her neonatal period was uneventful. There was no family history of a similar illness.
At the time of presentation, she also had raised multiple reddish rashes involving the posterior neck, left lower jaw, left buccal area and left border of her tongue. These lesions were said to have been noticed about two days after birth and have only sightly increased in size since their appearance. There was no bleeding either from the lesions or any other part of her body; neither did she have swellings in any other part of her body. On examination, she was well nourished (weight – 7 kg) and alert, but in respiratory distress with intercostal and subcostal recessions, respiratory rate of 36 breathes per minute and SPO2 of 98% in room air. She had biphasic stridors worse during inspiration. Chest auscultation revealed equal air entry bilaterally with transmitted sounds. There were multiple plaques of various sizes in the locations stated in the history. These lesions were soft and non-tender, with the largest measuring 5 × 3 cm in its widest diameter on the left lower jaw.
A diagnosis of infantile haemangioma in the ‘beard’ distribution with upper airway involvement was made. Child was admitted and placed on intranasal oxygen via nasal prongs, intravenous hydrocortisone and oral propranolol at 2mg/kg/day (in 2 divided doses). Chest radiograph upon admission showed no changes. Her full blood count and differential count results were normal. Patient showed modest response to treatment as the respiratory distress subsided and the stridor markedly reduced in intensity. However, no changes were noticed in the cutaneous haemangioma prior to her discharge on oral propranolol after five days of admission. Before discharge, her caregiver was counselled on the disease as well as the need for compliance to follow-up and medication.
At one week follow-up, she did not have respiratory distress but had slight stridor only while crying and suckling on the breast. After one month, during her follow-up, patient had no stridor. The cutaneous lesions had markedly reduced. She was lost to follow-up thereafter.
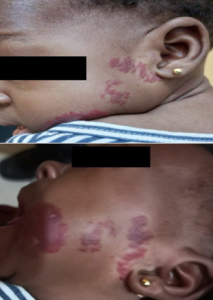
Figure 1. Showing a photograph of the 3-month-old female infant with segmental facial cutaneous haemangioma in the “beard” distribution.
DISCUSSION
Airway infantile haemangiomas constitute a rare occurrence and may be life threatening in the proliferative phase.1,9 It is during this early proliferative phase that patients become symptomatic, developing characteristic biphasic stridor, which may progress to respiratory distress.11 It’s rarity, alongside a mortality rate of about 50% when left untreated makes SGH to pose a great challenge to clinicians evaluating children for respiratory distress.5,11
Subglottic Haemangioma is often mistaken for more common conditions such as croup or bronchiolitis as also seen in our case.7,8,11 According to a retrospective case review by Sherrington et al, the correct diagnosis of airway haemangioma was made during the first admission only in 68% of infants.10 Although SGHs can occur in isolation, the presence of cutaneous haemangiomas, especially in the “beard” distribution may also suggest the presence of SGH in children with respiratory distress.7,11
In the case mentioned earlier the recurrence of her symptoms as well as the presence of segmental cutaneous haemangioma led to the suspicion of an airway involvement. Yet due to limited facilities in our centre as well as patient’s caregiver’s financial difficulties, we were unable to carry out some investigations such as direct laryngobronchoscopy and magnetic resonance imaging or magnetic resonance angiography of the head and neck. These would have aided in the determination of the extent of the involvement of the airway and confirmation of subglottic affectation.
Over the past few decades, treatment modalities for SGH have been evolving. These include topical therapies (corticosteroids, imiquimod, timolol), intralesional therapy (corticosteroids), systemic therapy (corticosteroids, interferon, vincristine) as well as carbon dioxide laser, tracheostomy, and open surgical resection.2,5,11 Systemic corticosteroids were the initial treatment of choice for a long time as about 30% of lesions respond to this method, but the child would be exposed to the negative adverse effects of systemic steroids.5,11 However, in 2008, Leaute-Labreze et al observed rapid regression of a large infantile haemangioma in a child who was being treated with propranolol for an unrelated infantile cardiomyopathy.12 Similar results were also observed within 24 hours of initiating propranolol treatment in 10 additional patients.12 Since then propranolol has become the new first line treatment for infantile haemangioma including airway haemangiomas.11,12
Although only seen in about 2% of users, most commonly encountered side effects of propranolol treatment include sleep disturbances and irritability. Other potentially serious but rare side effects include bronchospasm, bradycardia, hypotension, and hypoglycaemia.4,11 The exact mechanism of action of propranolol in haemangiomas is not known, but it has been speculated by authors to increase apoptosis and down-regulation of vascular endothelial growth factor as the result of vasoconstriction.2,4
Following diagnosis, our patient was commenced on oral propranolol at 2mg/kg per day (in 2 divided doses) and her vital signs as well as random blood sugar levels monitored closely at initiation of the therapy. Upon discharge the patient’s caregiver was instructed to administer propranolol orally after a meal to reduce the risk of hypoglycaemia. At her one week follow-up she had slight stridor only while crying and suckling on the breast. There was no respiratory distress. By one month follow-up, patient had no stridor. The cutaneous lesions had markedly reduced. Subsequently, she was lost to follow-up.
CONCLUSION
Obstructing airway haemangiomas are rare and, as such, missed or late diagnosis are not uncommon especially among primary health care givers. A high index of suspicion is thus needed for this condition in the young infants with respiratory distress or stridor presenting with cutaneous lesions. Anticipatory management of these airway complications may be necessary in resource poor settings to improve survival.
REFERENCES
- Imoudu IA, Yusuf MO, Ahmed H. Infantile haemangioma in the ‘beard’ distribution: a case report. Asian Oncol Res J. 2018;1(1):15-19.
- Maguiness SM, Frieden IJ. Current management of infantile haemangiomas. Semin Cutan Med Surg. 2010;29:106-114. doi:10.1016/j.sder.2010.03.009
- Krowchuk DP, Frieden IJ, Mancini AJ, Darrow DH, Blei F, Greene AK et al. Clinical practice guideline for the management of infantile haemangiomas. Pediatrics. 2019;143(1):e20183475.
- Kowalska M, Debek W, Matuszczak E. Infantile haemangiomas: and update on pathogenesis and treatment. J Clin Med. 2021;10:4631. https://doi.org/10.3390/jcm10204631.
- Rahbar R, Nicollas R, Roger G, Triglia J, Garabedian E, McGill TJ et al. The biology and management of subglottic haemangioma: past, present, future. Laryngoscope. 2004,114:1880-1891.
- Rosenblatt A, Mathes EF, Rosbe KW. Infantile hemangiomas: from pathogenesis to clinical features. Res Rep Neonatol. 2012;2:55-64.
- Oliveira JC, Azevedo I, Gonçalves A, Moreira C. Stridor is not always croup: infantile haemangioma in the airway. BMJ Case Rep. 2017;2017:bcr2017222449. doi: 10.1136/bcr-2017-222449.
- Alsaquoub SM, Almutairi SG, Bawazir SM, Alshiha WS, Halawani MS, Alshammari J. Subglottic hemangioma can be missed: two case reports. J Pediatr Surg Case Rep. 2019;51:1-4. Available from: http://doi.org/10.1016/j.epsc.2019.101308
- Corbeddu M, Meucci D, Diociaiuti A, Giancristoforo S, Rotunno R, Gonfiantini MV, et al. Management of upper airway infantile hemangiomas: experience of one Italian multidisciplinary centre. Front Pediatr. 2021;9:717232. doi:10.3389/fped.2021.717232.
- Sherrington CA, Sim DKY, Freezer NJ, Robertson CF. Subglottic haemangioma. Arch Dis Child. 1997;76:458-459.
- Hardison SA, Dodson KM, Rhodes JL. Subglottic hemangioma treated with propranolol. Eplasty. 2014;14. Available from: https://api.semanticscholar.org/CorpusID:5143985
- Leaute-Labreze C, Dumas de la Roque E, Hubiche T, Boralevi F, Thambo JB, Taieb A. Propranolol for severe hemangiomas of infancy. N Engl J Med. 2008;358:2649-51.
